What is GERD?
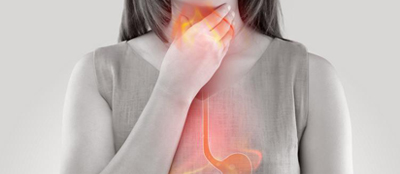
GERD that stands for Gastroesophageal Reflux Disease, often called Acid Reflux, is a long-term disease condition where stomach content (especially acidic content) refluxes or comes back to the mouth via the esophagus or the food tube, giving rise heartburn, acidic taste in the mouth, chest pain and even breathing problems among many. However, studies reveal that symptoms associated with GERD are more common (20 – 25%) among people living in Western countries (such as U.K.) as compared to those belonging to Asian countries (such as Malaysia) where it is limited to 10 – 15%.
What are the GERD symptoms?
The most common symptoms of GERD include HEARTBURN (even though it has nothing to do with the heart), strong acidic taste in the mouth, sore throat, swallowing problem, high rate of salivation and coughing.
Repeated GERD episodes often cause injury to the esophagus, resulting in:
- Reflux esophagitis – Necrosis (death of local cells) of esophageal epithelium causing ulcers close to the connection between the stomach and the esophagus
- Esophageal strictures – Narrowing of the esophagus caused by reflux-induced inflammation
- Barrett’s esophagus – Intestinal metaplasia (changes of the epithelial cells from squamous to intestinal columnar epithelium) of the distal esophagus
- Esophageal adenocarcinoma – A type of cancer
Even though some people claim GERD causing sinusitis, recurrent ear infection, as also idiopathic pulmonary fibrosis, these have not been medically established so far.
What causes GERD?
Gastroesophageal Reflux Disease is primarily caused due to the failure of the Lower Esophageal sphincter valve, thus allowing a part of the acidic stomach contents to travel back to the esophagus, creating all the issues stated above.
However, some of the following factors also contribute to the onset of GERD:
- Obesity – Increasing BMI is often associated with GERD to a large extent. With more than 2,000 people with symptomatic reflux disease, it has been proved that 13% of changes in esophageal acid exposure are attributable to changes in BMI.
- Hiatal Hernia hikes the likelihood of GERD on account of mechanical and motility factors.
- Zoollinger-Ellison Syndrome which can be found in increased gastric acidity due to gastrin production.
- High Blood Calcium level which also can heighten gastrin production, giving rise to higher acidity.
- Scleroderma and systematic sclerosis may cause esophageal dysmotility.
- Prednisolone (High consumption rate).
- Visceroptosis or Glenerd Syndrome in which the stomach has gone down in the abdomen, upsetting the motility and acid secretion of the stomach.
How GERD is diagnosed?
Diagnosis of gastroesophageal reflux disease is primarily based on the symptoms presented by the patient, as also the following tests and observations.
- A test to monitor the amount of acid in your esophagus – Ambulatory acid (pH) probe tests use a device to measure acid for 24 hours. The device identifies when, and for how long, stomach acid regurgitates into your esophagus. One type of monitor is a thin, flexible tube (catheter) that’s threaded through your nose into your esophagus. The tube connects to a small computer that you wear around your waist or with a strap over your shoulder.
Another type is a clip that’s placed in your esophagus during endoscopy. The probe transmits a signal, also to a small computer that you wear. After about two days, the probe falls off to be passed in your stool. Your doctor may ask that you stop taking GERD medications to prepare for this test.
If you have GERD and you need surgery, you may also have other tests, such as:
- An X-ray of your upper digestive system. Sometimes called a barium swallow or upper GI series, this procedure involves drinking a chalky liquid that coats and fills the inside lining of your digestive tract. Then X-rays are taken of your upper digestive tract. The coating allows your doctor to see a silhouette of your esophagus, stomach and upper intestine (duodenum).
- A flexible tube to look inside your esophagus. Endoscopy is a way to visually examine the inside of your esophagus and stomach. During endoscopy, your doctor inserts a thin, flexible tube equipped with a light and camera (endoscope) down your throat.
Your doctor may also use endoscopy to collect a sample of tissue (biopsy) for further testing. Endoscopy is useful in looking for complications of reflux, such as Barrett’s esophagus.
- A test to measure the movement of the esophagus. Esophageal motility testing (manometry) measures movement and pressure in the esophagus. The test involves placing a catheter through your nose and into your esophagus.
What are the modes of Treatment for GERD?
Treatment for GERD usually begins with over-the-counter medications that control acid. If you do not find relief within a few weeks, your doctor may recommend other treatments, including medications and surgery.
Over-the-counter treatments that may help control GERD symptoms include:
- Antacids that neutralize stomach acid. Antacids, such as Maalox, Mylanta, Gelusil, Gaviscon, Rolaids and Tums, may provide quick relief. But antacids alone won’t heal an inflamed esophagus damaged by stomach acid. Overuse of some antacids can cause side effects, such as diarrhea or constipation.
- Medications to reduce acid production. Called H-2-receptor blockers, these medications include cimetidine (Tagamet HB), famotidine (Pepcid AC), nizatidine (Axid AR) or ranitidine (Zantac). H-2-receptor blockers don’t act as quickly as antacids do, but they provide longer relief and may decrease acid production from the stomach for up to 12 hours. Stronger versions of these medications are available in prescription form.
- Medications that block acid production and heal the esophagus. Proton pump inhibitors are stronger blockers of acid production than are H-2-receptor blockers and allow time for damaged esophageal tissue to heal. Over-the-counter proton pump inhibitors include lansoprazole (Prevacid 24 HR) and omeprazole (Prilosec, Zegerid OTC).
Postscript:
GERD is best controlled by leading healthy lifestyle, reducing or cutting down alcohol consumption as also giving up smoking for good. Over and above, consumption of fried and/or fatty food should be eliminated totally. And as a last reminder – Do not indulge in drinking Champaign.