

Subho Noboborsho from LivGastro.
We wish you more happiness and excellent health throughout the year.
Celebrations are mirrored in grand feasts that define culture, heritage, and so much more. Who can know it better than Bengalis? However, if you are someone aged above 50 and seem to be alienated from these joys due to worries of heartburn or indigestion, you can still embrace better gut health by adopting mindful habits and preventive healthcare.
At LivGastro, we believe that understanding the subtle shift from “functional discomfort” to “organic pathology” is the key to longevity. As the premier gastroenterology specialist in Kolkata, we see firsthand how proactive clinical intervention can prevent life-altering diagnoses.
So let’s delve deeper than just high-fibre foods and hydration tips to gain a clinical understanding of what actually changes in your gut after 50. Which ordinary symptoms deserve extraordinary attention, and why preventive gastroenterology and other considerations matter.
The gastrointestinal tract does not age in isolation. After 50, several physiological changes converge:
Simultaneously, the risk of structural changes such as polyps, diverticula, and mucosal lesions begins to rise sharply. What this means clinically is that symptoms which were once minor for a 30-year-old person may carry more suggestive diagnosis reports than someone over 50-years of age. The same symptom; a very different clinical story.

The “minor” levels of recurrent issues are where clinical judgement diverges most sharply from popular health advice. Here are some of the most commonly dismissed symptoms among patients over 50 and the serious conditions they can conceal.
Preventive gastroenterology is not about running every test available. It is about the right test, at the right time, for the right patient. Here is what current evidence and American College of Gastroenterology guidelines recommend for adults in this age group:
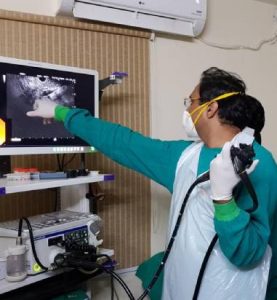
If you or a family member has been experiencing persistent or unexplained digestive symptoms, we invite you to consult Dr. Vijay Kumar Rai (DM – Gastroenterology, Fellow of the American College of Gastroenterology, Fellow of the American Society of GI Endoscopy) at either of our Kolkata centres – Beleghata or Dhakuria – or reach us via telemedicine from anywhere in Bengal.
Appointments: +91 9147105221 | WhatsApp: 9369120028 Clinic hours: Monday to Saturday, 9 AM – 1 PM and 4 PM – 8 PM. Book an Appointment at livgastro.in.
Current international guidelines recommend colonoscopy screening starting at age 45 for average-risk individuals, and earlier if there is a family history of colorectal polyps or cancer. The critical point is that colorectal cancer is often entirely asymptomatic in early, highly treatable stages. Waiting for symptoms to appear before seeking a colonoscopy is clinically counterproductive. The purpose of a screening colonoscopy is precisely to act before symptoms develop.
Yes — particularly if symptoms persist or intensify. Long-term undiagnosed reflux can be hazardous over time. Prolonged unsupervised antacid and PPI use also carries its own metabolic risks. A one-time specialist consultation can clarify whether your symptoms require investigation or simply optimised management.
Significantly, yes. A general physician manages a broad spectrum of conditions and is best suited for initial assessment. Consulting a gastroenterology specialist in Kolkata, who is qualified with additional years of superspecialty training, helps get straight to the treatment without multiple referrals. The diagnostic workup is appropriately targeted.
While benign explanations exist, new-onset reduced appetite, unintentional weight loss, and abdominal bloating can be early indicators of upper GI malignancy, pancreatic pathology, or hepatic disease—conditions whose early detection makes a direct difference to treatment outcomes. Please do not attribute these symptoms to ageing without a proper specialist assessment.
The liver, bile ducts, and pancreas are all part of the hepatobiliary system, which falls squarely within the domain of gastroenterology and hepatology. Symptoms such as jaundice, pale stools, dark urine, upper right abdominal pain, persistent fatigue, or abnormal liver function tests all require the same specialist. At LivGastro, Dr. Vijay Kumar Rai manages the complete spectrum — from oesophageal disorders and peptic ulcer disease to liver cirrhosis, biliary obstruction, and pancreatic disease — ensuring that interconnected organ systems are evaluated together, not in isolation.

As a leading gastroenterology clinic in Kolkata, we at Livgastro widely diagnose cases w
read more
Don’t Panic! For team LivGastro is here to offer their unparalleled DAY CARE services A
read more
Acidity and liver disorders are two common health issues that can affect anyone. While a
read more